Last Updated on June 24, 2022 by Laura Turner
Emergency medicine draws many students towards it because of the lifestyle-friendly aspect, shift work, and variety of procedures that a physician in the emergency department (ED) performs.
The thread ED Procedures for Med Students is an excellent resource that mentions some of (if not most) of the procedures that most ER physicians would expect a medical student to be familiar with or be asked to perform on a rotation, in no particular order.
All of these procedures can be searched for on Google or YouTube where you can find instructional videos on how-to, indications, contraindications, and more!
- Splinting
Basic splinting (OrthoGlass, Plaster, SAM splint, etc) is indicated for orthopedic injuries and at other times when the integrity of the extremity is compromised or otherwise should have limited mobility (fractures, soft-tissue trauma, gout, etc.).
- Laceration Repair
Laceration repair can be accomplished in a few different ways. Sutures, staples, and Dermabond are a few options that are available. Depending on the size, complexity, location, and reparative needs of the wound, provider discretion is often used to choose the repair method.
- Intravenous (IV) access and Ultrasound (US) guided IV access
IV access is established in order to administer medications, fluids, and blood products. US guided IV access is utilized when an appropriate vein (too small of a diameter or inadequate location) cannot be visualized or palpated.
- Intraosseous Access (IO)
Intraosseous access (IO) is often obtained when a peripheral line is unable to be obtained on a critical patient or during a code/peri-code situation. IO access can be established in various locations (depending on the age of the patient) and is found to be more successful than peripheral IV access.
- I&D
Abscess Incision and Drainage (I&D) is a procedure that is performed for areas of cellulitis which have become infected. Utilizing a scalpel, an incision is made in the abscess and the contents are drained. An optional step is to pack the wound with iodoform (antibiotic soaked gauze), but this is up to provider discretion.
- Arthrocentesis
Arthrocentesis (synovial fluid/joint aspiration) is used to drain synovial fluid from the joint capsule to relieve pain, pressure, or to perform laboratory testing if an infection is suspected.
- Lumbar Puncture
Lumbar puncture (LP)/spinal tap is a procedure where a spinal needle is inserted between vertebra into the spinal canal to obtain a sample of cerebrospinal fluid for laboratory testing. Lumbar punctures can be used to rule out conditions or differentiate between disease pathologies that are similar. Some of the reasons that a LP may be performed are to test for meningitis, underlying disease processes in migraine sufferers, or other neurologic conditions.
- Chest Tubes
Chest tubes are placed to drain blood, air, or other fluid from the pleural cavity. This is often an emergent procedure that is performed on a critical patient in the emergency room. Trauma, infection, cancer, or a spontaneous pneumothorax are some of the indications for the insertion of chest tube.
- NG/OG Tubes
Nasogastric/Orogastric (NG/OG) tube insertion is a tube that is placed through the nose (naso-) or mouth (oro-) into the stomach to drain fluid (suction), administer medication, or food. Naso/orogastric tubes can also be used to take a sample of gastric contents for laboratory testing (for example, in the case of gastrointestinal (GI) bleeding).
- Intubation
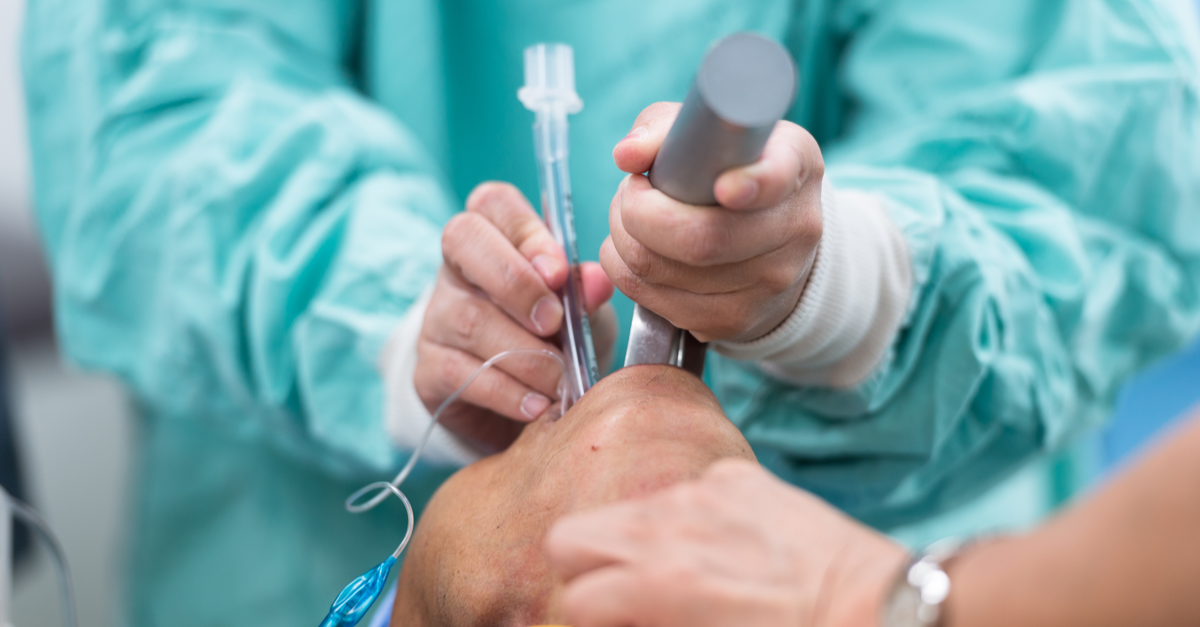
Endotracheal Intubation is a procedure that is performed when the airway, airway reflexes, or the gag reflex is compromised. There are a few ways to perform this procedure. Direct laryngoscopy (DL) is performed with a laryngoscope and allows for direct visualization of the vocal cords. Video laryngoscopy (VL) is another option which allows the provider to see the vocal cords indirectly on a monitor/video screen. Intubation provides protection from aspiration in the case of vomiting, unconsciousness/compromised airway reflexes, or severe injury/illness. In the event that the patient does still have present airway/gag reflexes, a procedure called Rapid Sequence Intubation (RSI) can be performed. RSI involves sedation and subsequent paralysis of the patient in order to safely secure the airway with an endotracheal tube.
- ABG
Arterial Blood Gas (ABG) is often obtained in patients who are experiencing respiratory compromise or are otherwise very ill. An ABG is drawn by inserting a needle attached to a syringe containing heparin into an artery. An ABG can give the provider specific information about perfusion status and includes specific values of pH, PaO2, PaCO2, SaO2, and HCO3-.
- Arterial Line Placement
Arterial line placement is a procedure which is performed by placing a catheter into an artery (usually the radial or ulnar artery) in order to measure arterial blood pressure or obtain blood samples for laboratory testing.
- Foley Catheter Placement
Foley catheter placement is a procedure that is performed in order to relieve the urinary bladder. A catheter is placed via the urethra and is passed into the urinary bladder. These devices are often placed to measure urinary output or relieve urinary retention.
- Paracentesis
Paracentesis is a procedure that is performed to remove fluids from a body cavity, similar to how a chest tube allows fluid or blood to be removed from the chest cavity. An example of this procedure would be to relieve ascites (fluid collection in the abdomen) that results in a distended abdomen.
- Digital Nerve Block
Digital nerve block is utilized when there is trauma or infection of a digit. While there are a few variations in which this procedure can be performed, these are again, provider specific. Digital nerve blocks consist of injecting an anesthetic into the general area surrounding the digit in order to provide anesthesia to the area being examined/repaired.
- Nasal Packing
Nasal packing is performed for uncontrolled epistaxis (nose bleed). Nasal packing is often performed using a commercial device that is used to place compact cotton in a posterior direction in order to control bleeding.
Hopefully this article provided a quick overview of some of the procedures that you will get to witness–and possibly perform–when rotating through the emergency department. What are some procedures that I did not include that you think are important for others to know about? Post your suggestions in the comments below.
Websites that you might find helpful: